Diffusing Health Innovations

Publications
Research Summary
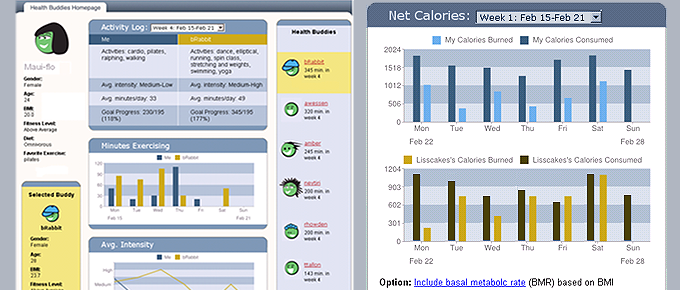
How does the composition of a population affect the adoption of health behaviors and innovations? To understand how changes in people’s social “neighborhoods” affect the spread of health innovations, we developed an in vivo study that manipulated the level of “homophily”—similarity of social contacts—among the participants in an online fitness program. Previous theoretical work suggests that at the individual-level homophily can increase behavioral influence between contacts, however it can also create population-level barriers that force less healthy individuals to interact primarily with one another, thereby reducing their access to important new health innovations. As a result, an important network-level effect of homophily is that the people who are most in need of a health innovation may be among the least likely to adopt it. To study how homophily affects the dynamics of novel health behaviors reaching less healthy individuals, we created the “Health Buddies program” within the “GetFit” online exercise program. Our design created large, interconnected peer-to-peer fitness networks, and rearranging the social relationships among the participants based on Age, Gender and BMI. To study the effects of these relationships on participants’ adoption of new health technologies, we created a novel online dieting tool (called a “diet diary”) and introduced it into each of ten independent health communities.
 The results showed that social similarities, or “homophily” on health characteristics significantly improved adoption both in the overall population, and also among the obese members of each of the communities. These highly significant findings imply important new directions for implementing online social network configurations to impact health outcomes. Our findings suggest ways in which specific groups might be targeted to improve behavior change. They further suggest ways in which networks might be rearranged explicitly to create more conducive environments for social spreading of health innovations. Building on these results, we our current studies are extending this environment to investigate related questions such as: how do these networks evolve endogenously? Who are the most influential members of the network? Are social influences on exercise and diet behavior the same as those on smoking cessation and vaccination compliance? And, how do structures of social interaction affect the spread of sentiment toward prophylactic health behaviors, such as preventative screening and vaccinations?
The results showed that social similarities, or “homophily” on health characteristics significantly improved adoption both in the overall population, and also among the obese members of each of the communities. These highly significant findings imply important new directions for implementing online social network configurations to impact health outcomes. Our findings suggest ways in which specific groups might be targeted to improve behavior change. They further suggest ways in which networks might be rearranged explicitly to create more conducive environments for social spreading of health innovations. Building on these results, we our current studies are extending this environment to investigate related questions such as: how do these networks evolve endogenously? Who are the most influential members of the network? Are social influences on exercise and diet behavior the same as those on smoking cessation and vaccination compliance? And, how do structures of social interaction affect the spread of sentiment toward prophylactic health behaviors, such as preventative screening and vaccinations?
Funding
Research on this project was supported by an M.I.T. Computers and Communications Award granted to PI Damon Centola. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Massachusetts Institute of Technology.
